Pain is among one of the most usual factors individuals call an ambulance. In the rear of a relocating car, with tools rattling and no guarantee of a quick healthcare facility handover, the criterion you embed in those very first minutes shapes the patient's trajectory. The unit PUAEME008 Give Pain Administration outfits -responders to examine, treat, and re‑assess pain safely in the pre-hospital context. It blends medical judgment with operational self-control. The end results are concrete: less call for help on scene, smoother extrication, much safer transportation, and enhanced individual fulfillment. For several medical professionals, it likewise functions as a foundation enter more comprehensive pain monitoring programs and certificate paths that branch out method past emergency care.
This overview unpacks the skills, assessments, and results that PUAEME008 expects. It connects those assumptions to day-to-day work, and it points to practical training routes, whether you are a paramedic in a rural station, a nurse relocating into event medication, or a physiotherapist looking for proficiency in emergency situation pain administration for sporting activities insurance coverage. The emphasis stays on what actually works when time is brief and the photo is messy.
What PUAEME008 Covers and Why It Endures
The unit sits within public security and emergency monitoring training plans in Australia. Its range is deliberately sensible: safe, prompt, and ethical administration of pain relief in the area. Graduates should have the ability to assess discomfort, select the ideal method, provide within scope, display result, and escalate when required. The system sustains carriers that may encounter a kid with a broken forearm at a sporting activities oval, a farmer with a crush injury in a shed, or an older grownup with a hip fracture on a chilly washroom floor.
It is not a pharmacology lecture disguised as an expertise. You will certainly learn analgesic alternatives relevant to your scope, but you invest as much time on person analysis and setting control as on application charts. The toughest experts end up being ingenious at accumulating the minimal information needed to act without missing red flags. They maintain methods at their fingertips, yet they customize to the person before them.
PUAEME008 also works as a bridge. Numerous that complete it later on seek a pain monitoring certificate training course or pain administration accreditation that expands to chronic and step-by-step pain. Others sew it right into a mosaic of short training courses suffering administration and advanced life assistance, creating a profile that fits event health, extracting websites, or access solutions. Due to the fact that the system straightens with a narrow yet crucial piece of care, it maintains its value across settings.
Assessing Pain When Time and Room Are Tight
The analysis series is more than a scale. It is an organized conversation, aesthetic scan, and quick physical examination that records both the extent and the pattern.
You beginning with the patient's words. Ask open, after that focused concerns: Where is the pain, what does it feel like, when did it begin, what makes it worse or far better? If you are making use of a numerical ranking range, set context. I will ask you to rate your pain from absolutely no to 10, where absolutely no is no discomfort and ten is the most awful you can envision. Also knowledgeable medical professionals avoid this sentence, and people react with a number that does not match their interior yardstick. In children, usage faces scales or basic descriptors. In nonverbal grownups, sew with each other taking a breath pattern, articulation, face stress, muscular tissue safeguarding, and important sign trend.
You associate the tale with visuals and palpation when suitable. Search for asymmetry, defect, strained compartments, pallor, cyanosis, and swelling that developments throughout your time on scene. Relocate joints proximally and distally only if it does not worsen injury. Think about a secondary study when the mechanism recommends surprise injuries. I as soon as treated a patient that infatuated on surface forearm discomfort after a fall, just for a fast hips rock and leg-length check to reveal a much more severe hip injury. The pain they report is not constantly the pain that will certainly eliminate them.
Vital signs issue, however they can misguide. High blood pressure and tachycardia can mirror discomfort, fear, or hypoxia. Alternatively, a well-conditioned athlete may show very little adjustment regardless of extreme discomfort. Informed pattern recognition helps: a groaning individual with a stiff abdomen and a heart rate increasing from 90 to 110 frequently needs quick transportation and careful analgesia, not expanded probing.
Consciousness and cognition belong to the assessment. A head-injured patient who can not track a simple discussion can not accurately self-report. Readjust your analysis strategy and recruit a caretaker, yet avoid letting 3rd parties overwrite the person's own understanding if the individual has the ability to communicate.
Pharmacological Options Within Scope
The system recognizes that extents vary. A basic -responder may have dental or inhaled choices; sophisticated providers might carry IV or IO representatives. The task is not to memorize every medicine on the market, however to master risk-free use of those you carry.
- Methoxyflurane: A staple in several pre-hospital sets for modest to extreme discomfort, specifically bone and joint injuries. Fast start, non-invasive, and patient-controlled breathing. Key teaching factors include avoiding too much exposure throughout long term usage, ensuring sufficient ventilation in constrained areas, and preventing usage where malignant hyperthermia risk or substantial renal impairment is thought. For distressed people, the act of holding the inhaler includes a feeling of control that typically alleviates the total distress curve. Oral analgesics: Paracetamol and NSAIDs remain workhorses for mild to modest discomfort if the person can ingest and has no contraindications. Splinting plus oral analgesia can decrease transportation pain for basic fractures. Watch for timing, advancing dosage with person's self-medication, and NSAID warns in kidney condition, peptic abscess, and hemorrhaging risk. Nitrous oxide/oxygen mix: Useful for procedural pain like manipulation or extrication. It needs tools checks, correct scavenging, and attention to individuals with pneumothorax or digestive tract obstruction where gas growth offers threats. The brief half-life enables quick reassessment after the procedure. Opioids: Morphine and fentanyl are common at advanced degrees. They remain reliable for serious discomfort when titrated to result, especially in injury. The pre-hospital context boosts the importance of airway vigilance, cumulative sedation with alcohol or benzodiazepines, and step-by-step application with clear endpoints. Fentanyl's hemodynamic security often makes it a favored selection in hypotensive injury. In older grownups, start with smaller increments and extend your review intervals a touch longer. Ketamine: In innovative procedures, low-dose ketamine provides strong analgesia with very little breathing anxiety. It radiates in hypovolemia, burns, and entraped people. Appearance sensations are uncommon at analgesic doses yet can be alleviated with silent coaching and, if scope permits, a little benzodiazepine complement. Avoid the temptation to rush the dose; a sluggish press over a number of mins smooths the ride.
The heart of PUAEME008 is safety and security. Whatever representative you pick, verify 5 civil liberties, check for allergies and considerable comorbidities, file set numbers where called for, and display oxygenation, ventilation, perfusion, and mental status. Never allow a syringe secure your interest greater than the client's breast rise and fall.
Non-Pharmacological Measures That Outperform Their Reputation
An unexpected amount of discomfort yields to standard actions that need no prescription. Stiff splinting for long-bone fractures, sling and swathe for shoulder injuries, gentle grip and positioning within extent, and extra padding bony prestiges all matter. With burns, very early air conditioning with awesome, not cold, water for approximately twenty mins improves pain and outcomes, however do not delay transportation for prolonged air conditioning on deep or considerable burns.
Positioning stays a powerful tool. Individuals with abdominal discomfort often favor knees bent. Chest pain individuals usually pick a semi-Fowler placement that alleviates lack of breath. Regard their picked stance unless it disputes with various other top priorities like spine protection.
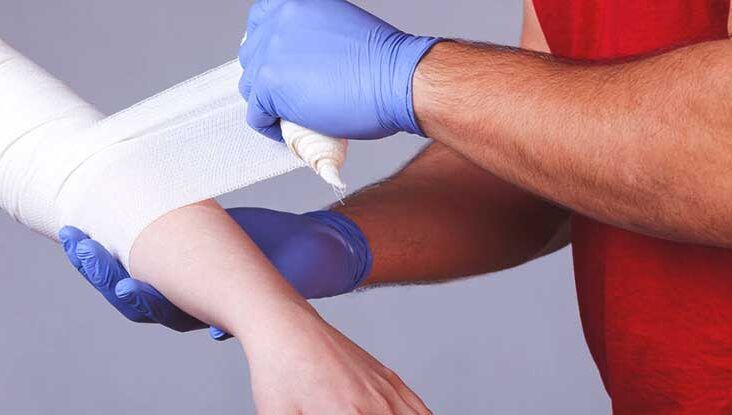
Psychological assistance modifications physiology. Speak in consistent tones, set expectations, and narrate your actions. On a country roadway after a rollover, I invested 2 minutes explaining specifically what the splint would certainly feel like as I used it. The person's respiratory price alleviated from 28 to 20 prior to we touched the arm or leg. PUAEME008 deals with such interaction as a proficiency, not a soft add-on.
Cold and heat treatments depend on the injury. Ice decreases swelling and discomfort in severe strains and pressures, preferably wrapped to avoid skin injury. Heat can help muscular tissue spasm, however avoid it in severe trauma or where swelling is developing.
Special Populaces, Refined Differences
Children analyze pain with family cues and atmosphere. A moms and dad's face will matter greater than your uniform. Get down to eye level, show the mask or inhaler initially, and allow them touch non-threatening tools. Dose drugs on weight, not age, and confirm numbers with caretakers and your reference. Step-by-step pain rises considerably in kids, so strategy analgesia prior to cannulation or fracture manipulation. Think about that dehydration accelerates medication impacts and adverse effects. Reassess commonly and record actions, not simply numbers.
Older adults present a different obstacle. They might under-report pain or stabilize it. Polypharmacy and comorbidities raise threat. Review for ecstasy and cognitive impairment. Avoid opioid stacking with existing sedatives, and titrate slowly. For hip fractures, gentle positioning and grip, plus a warmth pack to the back region for muscle relaxation, can conserve an opioid dose or 2. In the visibility of renal disease, be wise with NSAIDs.
Pregnancy complicates pharmacology and positioning. Lateral tilt past mid-second trimester safeguards venous return. Numerous services prefer fentanyl or low-dose morphine over NSAIDs in late pregnancy. Abdominal discomfort in pregnancy deserves a reduced threshold for transport and consultation.
Patients with material use problems should have the very same rigor as any person. Avoid stigmatizing language. Titrate to impact, record objectively, and maintain safety and security with positioning and monitoring. Blended drunkenness with alcohol can mask hypoventilation, so establish a high bar for pulse oximetry and capnography where available.
Scene Monitoring and Staff Coordination
Emergency discomfort monitoring does not take place in a vacuum cleaner. The unit anticipates you to incorporate analgesia with scene safety and logistics. If extrication is pending, plan your analgesic home window so pain alleviation peaks throughout motion. On pain management certification a steep driveway with a fragile shoulder dislocation, we adjusted timing so methoxyflurane reached effect right as the individual transitioned to the scoop stretcher.
Agree on roles. One medical professional manages the airway and keeps an eye on sedation degree. The other communicates dosing out loud and records. Closed-loop interaction stops dual application, particularly when syringe swaps occur under stress and anxiety. Alert obtaining centers to drugs provided, timing, and impact so they can improve your plan as opposed to repeat or reverse it.

Equipment checks are not busywork. A missing out on mouthpiece, an empty nitrous cylinder, or a dead suction battery can thwart good purposes. Many teams make use of brief responsive checks at change begin: turn the shutoff, really feel the circulation, click the capnography cable, press the bag. Pain administration training courses typically build these regimens right into simulation scenarios to make them automatic.
Documentation that Informs the Story
A crisp story supports individual security and lawful defense. Graph first pain descriptors, range ranking, and location. Create what you offered, just how much, when, and why you picked it. Include non-pharmacological procedures, person positioning, and splinting approach. Reviews need to review like a timeline: 14:12 fentanyl 25 mcg IV, 14:16 discomfort 8 to 6, RR 18, SpO2 98 percent on 2 L. Stand up to need to document just numbers. Actions, face, and function supply richer detail. Person able to birth weight with support at 14:29 carries more meaning than an only score.
When pain remains refractory, note what you eliminated and your acceleration steps. If you spoke with clinical control or elderly medical professionals, list their assistance. In multi-agency events, share a recap with on-scene supervisors to avoid therapy gaps.
Training Pathways: From Unit Proficiency to Certification
Many carriers start with PUAEME008 as a targeted stepping stone. It gives a practical toolkit you can make use of the following shift. From there, people diverge based on duty and interest.
- Pain monitoring training for registered nurses: Registered nurses in immediate treatment, perioperative settings, or remote facilities typically include sophisticated assessment, step-by-step analgesia, and titration methods. Pain management programs for registered nurses in some cases include modules on multimodal treatment and opioid stewardship customized to nursing range. Certification programs may stack PUAEME008 with wound care, IV therapy, and sedation competencies. Pain monitoring programs for physiotherapists: Physios who cover sporting activities occasions or job together with emergency teams gain from acute pain structures, splinting, and non-pharmacological techniques. These pain monitoring training courses appreciate the physical rehabilitation extent while showing clear reference sets off. Combination with concussion and spine analysis components is common. Provide discomfort monitoring course for pre-hospital practitioners: Ambulance services and event medication suppliers run brief programs in pain monitoring, usually straightened to PUAEME008 offer pain management. They concentrate on inhaled agents, nitrous, and opioid titration with extensive air passage surveillance. The better programs include nighttime and cramped-space simulations. Pain management certificate and qualification paths: If you intend to widen past severe treatment, try to find a certification program hurting monitoring that resolves intense, persistent, and cancer pain. A discomfort monitoring certification training course usually covers neurobiology, psychology of discomfort, functional analysis, and pharmacology across the continuum, plus interaction skills and moral factors to consider. Some programs acknowledge prior learning from PUAEME008 and shorten your path.
Not all discomfort administration programs are equivalent. Review training course hours, professors experience, simulation realistic look, and post-course assistance. Ask whether cases reflect your technique setting. I like programs that include failed-response scenarios and gray-zone choices, not simply textbook fractures.
The Skill of Titration and the Art of Timing
Titration divides certain suppliers from hesitant ones. The goal is not absence of discomfort, but acceptable discomfort that maintains safety and security and function. For numerous trauma people, relocating from a 9 to a 4 or 5 lets you splint and transport without fogging the air passage. That balance takes dosages in little actions and pauses for impact. Fentanyl comes to a head quickly, ketamine a bit slower at analgesic doses, and dental agents lag by 10s of minutes. Your strategy needs to value these pharmacokinetics.
Timing matters as high as the total dosage. If you will bring a client down three flights, peak effect needs to get to the landing, not at the visual. For procedural actions like shoulder reduction, pick either fast titration of a short-acting representative or a ketamine analgesic dose with silent coaching, depending upon range and skill mix.
Beware dosage momentum. After two tiny doses yield just small gains, teams often leap to a big third dosage that overshoots. Persistence and reassessment avoid see-sawing between pain and oversedation. Usage capnography where possible. A refined higher creep in ETCO2 might be your first warning.
Ethical Grounding: Permission, Equity, and Opioid Stewardship
PUAEME008 expects you to obtain grant the degree feasible, even under stress. Discuss benefits and risks in ordinary language. A basic script jobs: I can give you a medicine through your capillary that need to reduce your discomfort in a few minutes. It can make you sleepy and sluggish your breathing a little bit, so I will certainly see you very closely. Is that okay? For breathed in agents, demonstrate and allow the person hold the tool when appropriate.
Equity matters. People from marginalized teams usually report receiving less analgesia for the very same injuries. Construct a habit of structured assessment and documentation to counter implicit prejudice. If your numbers and story warrant therapy, follow through irrespective of accent, age, or regarded stoicism.
Opioid stewardship in the pre-hospital area rests on titration, tracking, and handover clearness, not on withholding required analgesia. Your role is to alleviate intense suffering securely, not to set long-term opioid trajectories. Clear paperwork and communication sustain the obtaining group in intending following steps, consisting of non-opioid techniques and discouraging when appropriate.
Measuring End results That Matter
The easiest pen is the pain score pattern before and after therapy, however end results surpass a number. Expect enhanced resistance of needed motion, minimized anxiousness, secure vitals, and the lack of unfavorable events. In service audits, purposeful outcomes consist of the percent of eligible trauma patients who received prompt analgesia, average time to very first dosage, and the price of considerable breathing clinical depression per 1,000 managements. Numerous solutions also track patient-reported experience measures at follow-up. Comments like They told me what to anticipate and I felt looked after typically associate with better physiological trajectories.
For individual professionals, maintain an individual log. Note what worked, what really did not, and why. Patterns arise: application that is constantly slow, abilities that need refresher courses, or protocols that could utilize explanation. Bring these observations to training leads. Good pain monitoring training adapts based upon frontline feedback.
Common Risks and Practical Fixes
Two mistakes repeat. The first is treating the number, not the person. A young adult that rates discomfort at 10 however giggles with close friends might be using the scale in a different way or dealing well. Focus on function and actions as well. Can they relocate with support, or do they stiffen and secure at every motion?
The second is skipping the review. After the initial wave of analgesia, re-examine the damaged area et cetera of the body. Swelling may have progressed. A limited splint might need helping to loosen. That five-minute check avoids difficulties and makes improvements dosing.
Other side instances are worthy of attention. In thermal burns, stay clear of hefty dosages that cloud respiratory tract assessment. For stomach discomfort where surgical treatment is likely, modern-day evidence supports proper analgesia as opposed to the old concern of concealing indicators. Still, maintain cosmetic surgeons in mind and record findings plainly before and after therapy. In believed compartment syndrome, discomfort disproportionate and pain on passive stretch linger regardless of analgesia. Escalate early.
Building Skills Through Calculated Practice
Competency rises with repeating, yet arbitrary repetition is slow. Deliberate method presses discovering time. Produce micro-drills. Before each change, verbalize your methoxyflurane contraindications while you set the package. When you restock fentanyl, practice a three-step titration plan for a 70 kg grownup and a 40 kg older grownup. Pair with a colleague and critique each various other's approval scripts.
Simulation ought to feel like work. Lower the lights, add sound, and imitate the cramp in your shoulder as you stoop by a Homepage car seat. Run sequences where the individual does not reply to your initial strategy so you practice escalation without panic. Make use of a metronome for slow-moving ketamine presses to stop the too-fast hand that welcomes side effects.
Finally, invest in broader knowing. A pain administration certification or a structured discomfort administration program exposes you to the biopsychosocial model and multimodal strategies. Physio therapists will deepen non-pharmacological methods. Registered nurses will refine titration in step-by-step setups. Pre-hospital service providers will harmonize sedation scales with transport realities. The best programs deal with PUAEME008 as a support point and develop external with nuance.
The Benefit: Calmer Scenes, More Secure Transportations, Better Trust
The first time you lower a patient's 9 out of 10 to a workable 4 as you pack them, you really feel the area adjustment. Family members breathe. Staff participants quit seeing the clock and begin believing two continue. The patient remembers that adventure differently, and they are more probable to engage with care on arrival. Throughout hundreds of situations, this translates into less combative transportations, fewer failed procedures, and fewer negative events.

PUAEME008 Supply Discomfort Management instructs not only exactly how to push a medicine or apply a splint, yet how to orchestrate the little choices that make acute pain manageable without endangering security. It prepares you for the cramped areas and incomplete details that specify pre-hospital job. Pair it with proceeded pain administration training, seek comments, and maintain refining. The skill is worth the effort, and the outcomes show on every shift.